Clinical Presentation: F.N. is a 70-year-old male with current tobacco use, hypertension, and dyslipidemia. He reports right buttock pain with walking 50 feet that resolves with rest. He also has a diagnosis of right-sided sciatica. On physical examination, his right femoral, dorsalis pedis, and posterior tibial pulses are diminished.
Step 1: History and physical examination are suggestive of PAD.
- Risk factors: age > 65, current tobacco, hypertension, dyslipidemia
- Exertional leg symptoms: right buttock pain after 50 feet that resolves with rest
- Physical examination: diminished pulses
Step 2: Obtain ABIs/noninvasive physiologic flow studies.
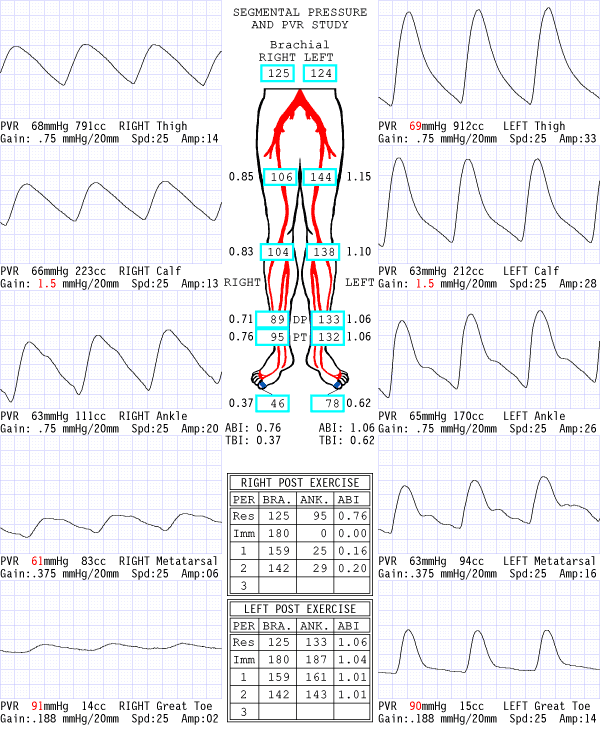
Interpretation: The right ankle-brachial index (ABI) is in the mild range. The pulse volume recordings are moderately abnormal on the right. The findings are suggestive of right iliofemoral disease. The significant post-exercise drop in ABI helps establish that the patient’s exertional buttock pain is more consistent with PAD rather than sciatica. The ABIs and PVR tracings on the left are normal. The PAD diagnosis is confirmed.
Step 3: Begin treatment for PAD.
The patient is started on optimal medical therapy and an exercise regimen but remains severely limited by his claudication symptoms after 3 months. Revascularization is being considered.
Step 4: Obtain additional anatomic assessment.
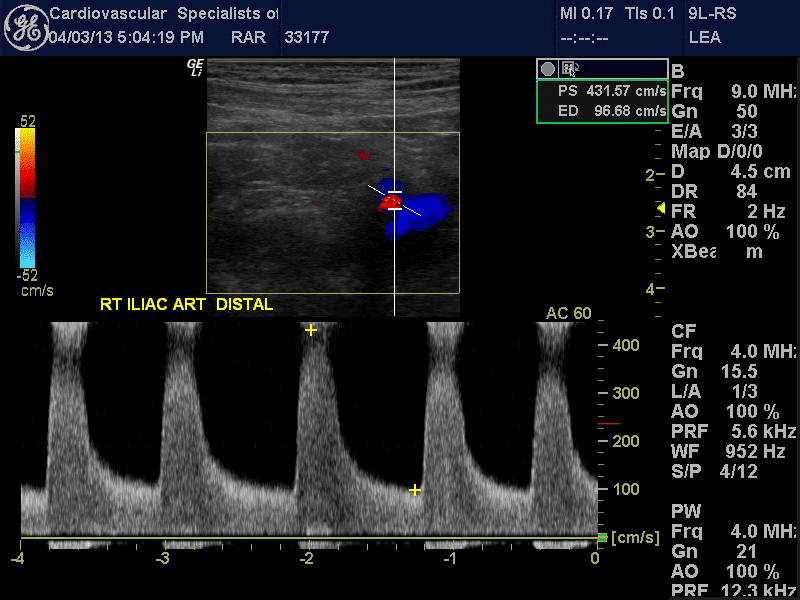
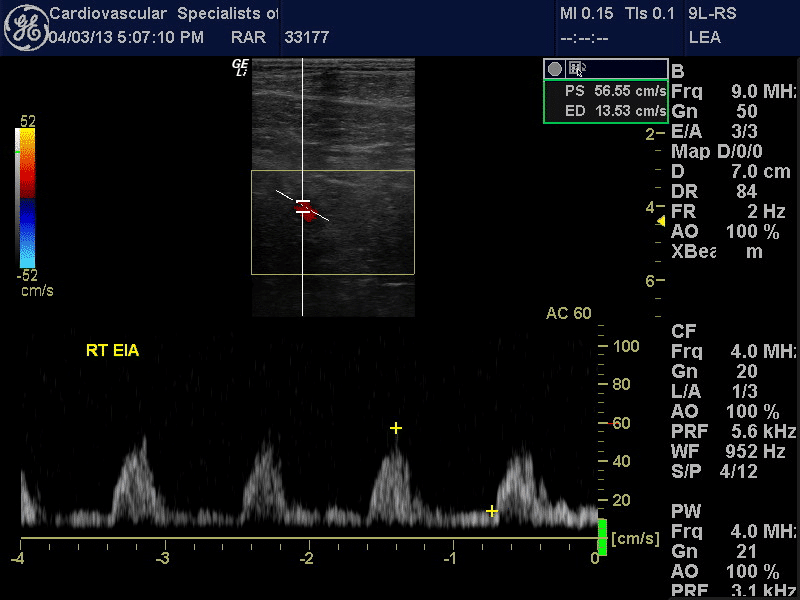
Arterial duplex image and spectral Doppler waveforms of the distal right common iliac/proximal external iliac artery indicate hemodynamically significant stenosis. The peak systolic velocity is markedly elevated at 432 cm/sec. The velocity ratio is elevated at 4.4. The spectral Doppler waveform of the distal external iliac artery is monophasic and demonstrates a tardus et parvus pattern. These findings are consistent with a significant distal common iliac/proximal external iliac artery stenosis.

Digital subtraction angiography image demonstrates high-grade stenosis of the right external iliac artery.
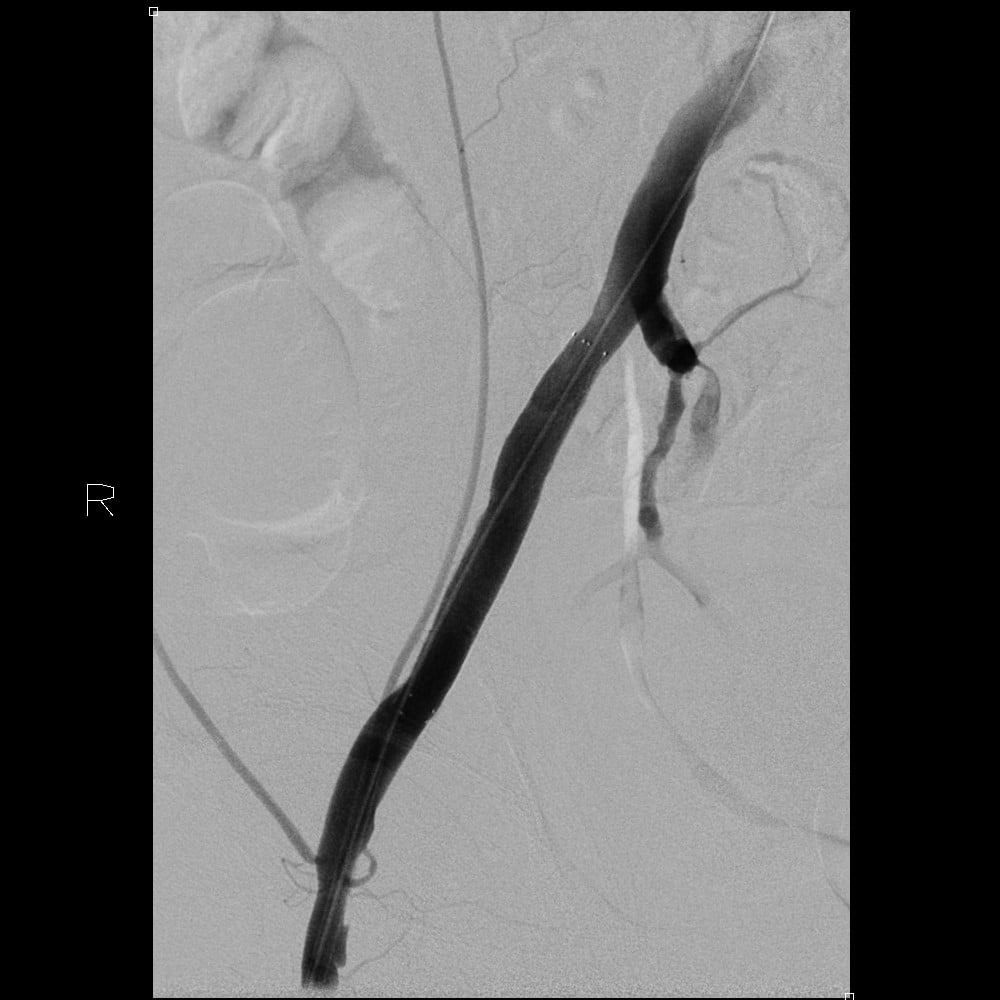
Digital subtraction angiography image of the right external iliac artery status post angioplasty and stent placement.

Noninvasive physiologic flow studies demonstrating normalization of ABIs and PVRs on the right following external iliac artery angioplasty and stenting.
